The Veteran Health Care Crisis
Our military personnel are subject to working and living conditions unlike any other workers, conditions that may be toxic to their health and—sometimes—to their families’ health as well. As Veterans, they bear both the visible and invisible wounds to prove it.
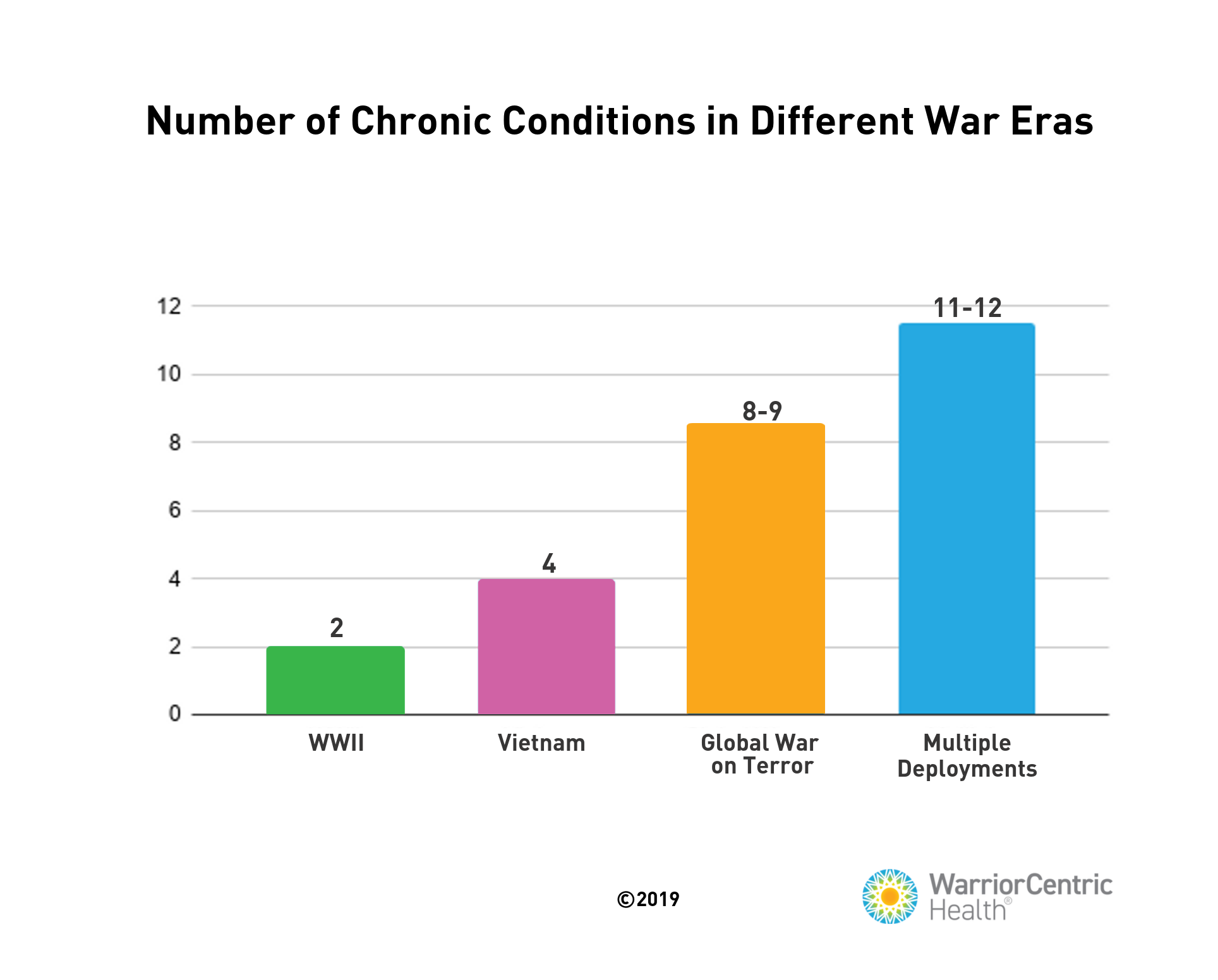
This is a simple fact: Young people enter the service as the healthiest of the healthy, but when they get out a few years later, most of them still in their late twenties or early thirties, about four out of five will report a chronic condition they didn’t have when they enlisted, even if they’ve never seen a battlefield.
And comorbidity is exploding.
The Veterans Administration Treats
Only a Fraction of the Warrior Community.
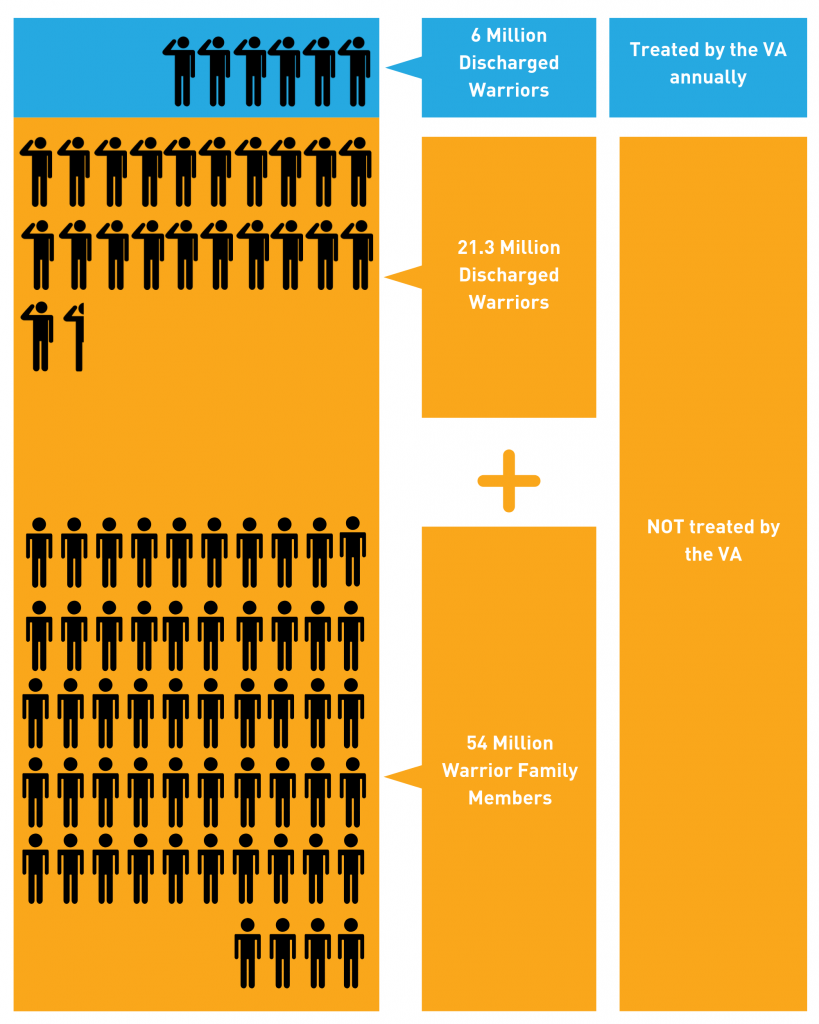
The VA’s mission is not to provide healthcare for ALL Veterans. In fact, only 12.2% of male Veterans and 20.6% of female Veterans solely use the VA for their healthcare in any given year. That leaves over 80% of Veterans who are getting their healthcare in the private sector, and virtually all of their family members. Many active duty service members, National Guard, and reservists also receive their healthcare from commercial facilities. Combined, this “Warrior Community” represents a significant portion of a commercial facility’s patient population—as much as 25%.
The vast majority of the Warrior Community is treated in civilian health systems.
The Private Hospital System is Not
Prepared to Treat the Warrior Community.
Most facilities are neither aware of this vulnerable and underserved population nor prepared to treat them optimally:
Only 57% of private hospitals screen for veteran status and only 10% utilize the data to identify care gaps.
![]() Their providers may lack the cultural competencies needed to communicate effectively with them.
Their providers may lack the cultural competencies needed to communicate effectively with them.
Military personnel are trained to “drive on”. Complaints and excuses are simply unacceptable. Veterans retain these (and other) elements of military culture, making diagnosis difficult for healthcare providers unaware of a patient’s Veteran status and ignorant of cultural cues.
The result? 25% of all Americans
Underserved by Their Healthcare Systems.
75 million individuals of the Warrior Community—roughly 25% of the total U.S. population—live their lives at substantially higher risk of multiple chronic health conditions than the general population. Yet they remain “invisible” to those systems, suffering in the shadows.
Meanwhile, many healthcare facilities struggle to improve outcomes for their patient populations, unaware of the opportunity within their walls.